Knowledge Hub 01: Introduction to Navigation and Survivorship
Learning Objectives
By the end of this Knowledge Hub, you will be able to:
- Define the goals and outcomes of cancer navigation and survivorship.
- Comprehend the domains of needs and phases for patients living with cancer.
- Explain the various roles of a professional or health navigation.
Introduction
This knowledge hub will introduce you to key concepts of cancer survivorship and navigation. Cancer is a very complex disease that is extremely difficult for patients and their families to navigate. People living with cancer undergo various domains of needs over their journey and require different levels of support throughout these phases. Navigation can be provided in multiple different ways with trained individuals all with the goal of patient engagement and participation in their care. This knowledge hub will discuss the ideology of navigation, survivorship and the associated principles (Cancer Fundamentals, 2019; Fitch, 2008).
1. Define the goals of navigation and survivorship
1.1 What is cancer?
Cancer is a broad term that describes the creation of damaged and over-proliferated cells in the body. These cells are deregulated and are not able to be controlled easily. Cancer can be caused by DNA damage via carcinogens and genetics, mutations from aging, chemicals, hormones or randomly (Cancer Fundamentals, 2019). Cancer can be caused in many different areas of the body such as breast, lung, prostate, colorectal, and many others.
1.2 Definition of cancer navigation
Cancer Navigation specifically is a role created to “help patients overcome healthcare system barriers and provide them with the timely access to quality medical and psychosocial care from before cancer diagnosis through all phases of their cancer experience” (Pfizer Oncology, 2018).
What are the roles of cancer navigation?
- Provides family-centered, ethical, safe care to clients with cancer and their families.
- Collaborates with the care team to gain a knowledge base of cancer diagnosis, treatments, stage and grading, and survivorship (Government of Northwest Territories, 2020). Provides educational information, resources, and references to ease the client’s cancer care journey (Government of Northwest Territories, 2020).
- Creates a therapeutic relationship with the client and their family (Government of Northwest Territories, 2020).
- Assists with the case management of the client’s cancer, assesses any problems that arise between the client and their family and evaluates interventions to support and follow up at appropriate times (Government of Northwest Territories, 2020).
- Creates and assesses interventions to curate a holistic healthcare approach tailored specifically to the client (Government of Northwest Territories, 2020). Refers the client to a higher level of care when and if needed (Government of Northwest Territories, 2020).
- Assesses the psychosocial, social, sexual, and spiritualistic needs of the client and uses an interdisciplinary approach to address any concerns.
- Gives clients and their families evidence-based information and teaching resources to supplement any concerns or questions regarding cancer and their care.
- Encourages credible and authentic educational materials appropriate to their learning level and readiness to learn (Government of Northwest Territories, 2020). Creates personalized education that is individualized to the client, which is specific to the needs of the client.
- Offers virtual and in-person education sessions to assist the client in their care plan.
- Works in collaboration with the individual health region following its policies, procedures, protocols and cancer team to support and evaluate the goals of the cancer navigation and their specific goals for their health.
- Works with the site of the clinic, doctors, hospital, and treatment centers to understand the goals of care (Government of Northwest Territories, 2020).
- Reports any issues within the healthcare system regarding their client to a higher level of management (Government of Northwest Territories, 2020).
- Promotes collaboration of a multi-disciplinary team to ensure services are not duplicated or missed.
- Educates the other members of the interdisciplinary team on the role of a navigator.
- Dissect the care plan to find gaps in services and make improvements (Government of Northwest Territories, 2020).
Refer to the Patient guide. http://www.bccancer.bc.ca/our-services/patient-guide
1.3 What are the goals of cancer navigation?
The goals of cancer navigation can be divided into five different objectives.
- Coordinating care: ensuring access to services in a timely fashion including procedures, doctor’s appointments, diagnostic tests, and any other necessary services (Pfizer Oncology, 2018).
- Education: This goal involves providing information and resources to develop the patient’s and family’s knowledge about cancer treatment, medications, and side effects, and create a basis for informed decision-making (Pfizer Oncology, 2018).
- Provide: The navigator should provide psychosocial support and comfort to the client, caregiver, and their families through the stages of their cancer journey (Pfizer Oncology, 2018).
- Identify: This goal revolves around the navigator’s skill to improve the client’s access to services and to identify gaps that are creating difficulty for the patient (Pfizer Oncology, 2018).
- Advocate: become an advocate for the patient and their family to ensure their concerns and their voice about their needs during their journey are heard and addressed (Pfizer Oncology, 2018).
For more information on the goals of oncology navigation, please see Figure 2 on page 17 of the Pfizer Oncology “Navigating the Cancer Continuum “document.
1.4 Introduction to survivorship and its factors
We need to know what survivorship means. According to the American Cancer Society (ACS) (2023a), survivorship refers to everybody who has had a diagnosis of cancer, regardless of where somebody is in their cancer journey. The National Research Council (2006) says survivorship has a different definition depending on who you are. Survivorship can be defined based on a timeline from diagnosis to treatment (National Research Council, 2006). A five-year relative survival rate refers to the percentage of people who are alive with the same grading and staging of cancer (American Cancer Society, 2023b).
The President’s Cancer Panel (2004b) notes that some view 5 years after diagnosis as being the mark of survivorship starting, while others do not even like to use the term survivor, instead they may seek other terms such as a fighter (as cited in, National Research Council, 2006). Mullan (1985) sees the period after treatment as being a time of extended survival (as cited in, National Research Council, 2006). During the period of extended survival, it is normal to be fearful of cancer coming back, to be tired and to have a loss of strength (Mullan, 1985, as cited in, National Research Council, 2006). Welch-McCaffrey et al. (1989) further explain that there are many pathways that survival can take (as cited in, National Research Council, 2006). You may find that the cancer comes back sometimes, there is a long period of no cancer, or a different type of cancer develops.
When your treatment is over it is important to know that everybody’s experiences will be their own (ACS, 2016). You may feel hope and fear, while another survivor has worry and happiness. You may feel so tired from your treatment, that a wave of emotions comes at you (ACS, 2016). It took time for you to adjust to your treatment, as it will take time to find what your new normal will be. The new normal according to the Government of Saskatchewan (n.d.) means the adjustment you will make after treatment has ended. You may want to start the routines again you had before treatment, or you want to discover what else life has for you (Government of Saskatchewan, n.d.). The Government of Saskatchewan (n.d.) has provided some examples of questions you may have after your treatment, including what your future energy levels will look like, and are there changes in daily routine will lower the risk of cancer returning. Other questions can be found by accessing the Government of Saskatchewan (n.d.) link. How your life before cancer was, may not fully be how it will be now, but you can make this adjustment (ACS, 2016). It is good to think positively, but it is also ok to embrace the emotions you are feeling, you don’t have to let others try to push positivity too much. The ACS (2016) explains that it is good to tell your loved ones how you feel, as our attitudes and thoughts do not cause cancer.
It is completely normal to focus on whether the cancer will come back, so much so that it stops us from being able to decide on simple things, and from falling asleep (ACS, 2016). Some people find that the thought of cancer can gradually disappear, with significant life events causing them to remember the uncertainty of their future. Please find strategies to help with uncertainty by using the ACS (2016) resource. Survivors can find that emotional support is a powerful way to help with the loneliness that comes with survivorship (ACS, 2016). The ACS (2016) has found in studies that when people can share how they feel, and learn new ways to cope, they can have better sleep, eat well and better quality of life. Support tools for connecting with counselling, spirituality, religion, getting better sleep and eating well can be found in these by using the ACS (2016) resource.
Managing your healthcare
Now that you have finished your treatment, you may have additional meetings with your oncologist, the specialist of your cancer (BC Cancer, n.d.a). Your care team may have a plan for you, so it is important to follow their advice. It is important to know that side effects will likely improve over time. If there are long-term side effects, your oncologist will be the person to ask about a plan. Even though you are done with your treatment, it is important to see your primary care provider, who may be your family doctor or nurse practitioner. They can assist you with any other health concerns (BC Cancer, n.d.a). The schedule of visits that you may have in the future is based on your needs, so it may look different than others (Government of Saskatchewan, n.d.). The treatment centre you receive treatment from can also provide information to any questions you have about side effects (BC Cancer, n.d.a). Please find their contact information by using the BC Cancer (n.d.a) link. Should you have questions outside of the treatment centre hours, 8-1-1 is the number for Health Link BC – Nursing Services. For those that are hearing impaired please call 7-1-1. If it is an emergency please call 9-1-1 (BC Cancer, n.d.a). It is important to tell your doctor about some specific symptoms.
See Queering Cancer. (n.d.). https://www.queeringcancer.ca/a-gift-too-hard-to-walk-away-from-the-sexual-and-gender-diversity-in-cancer-care-program/
What should I talk about at my follow-up?
When you sit down with your family care provider tell them how you feel (Canadian Cancer Society, 2018). Tell them the truth, they need to know about your thoughts and feelings to help you, even if they do not specifically ask about the symptoms you are having. If there have been some symptoms worrying or bothering you tell them. Your doctor may talk about some tests they would like done. It is ok to ask a family member or a friend to come with you for support (Canadian Cancer Society, 2018).
What will my follow-up care plan look like?
There will be visits to your oncologist and your family care provider. But what kind of information should you be talking about, and what is your role in your care plan? The Canadian Cancer Society (2018) says it is helpful to keep track of what goes on in your care plan. This can mean gathering information from the treatment centre you were at, which may have a cost. Having all of your health documents organized in a folder is a good start. Having all of the information on your diagnosis and treatment plan will help you and your doctor in the future (Canadian Cancer Society, 2018). It would be hard to remember every detail in your care plan without being able to look information up. Create a schedule to show when your future visits are, what tests you may have to do, what side effects experienced and your doctor should discuss, and what your wellness plan should look like to keep you healthy (Canadian Cancer Society, 2018).
What is maintenance therapy?
Part of your plan may be to have maintenance therapy, which is where drugs or hormones can be given to you for a longer time after your treatment (Canadian Cancer Society, 2018). Your care team wants to make sure that the cancer does not come back. It might make you feel that you have not yet reached the end of treatment. For others, it could be a relief to stop cancer from returning, or it may be a daily reminder of the medication you need. You might find it helpful to think of your maintenance therapy as another condition like diabetes or asthma that has to be cared for (Canadian Cancer Society, 2018). The American Cancer Society (2020a) resource has a lot of information about why mammograms are done, what happens during a pelvic exam, how to be prepared for your upcoming doctor’s visit, and why certain tests such as bone density tests are done. The link for the American Cancer Society (2020a) also has topics that focus on how to reduce the risk of cancer returning and second cancers.
What are the long-term effects of cancer treatment?
According to the Canadian Cancer Society (2018), long-term side effects are the side effects that continue past the end of your treatment. Some side effects are called late effects, which are side effects that start after the end of your treatment. We will explore some of the side effects you may be experiencing, but a complete list can be found by using the link for Canadian Cancer Society (2023v). We will also talk about how you can prevent these side effects from happening, or how to handle the ones that you are experiencing.
Side effects signal a return of cancer
Cancer that has returned is also known as a reoccurrence or secondary cancer according to Cancer Care Alberta (2022). Use the link for Cancer Care Alberta (2022) to see what symptoms that may indicate cancer has come back. If you do notice these symptoms tell your healthcare provider.
What is Second Cancer?
The American Cancer Society (2020c) explains a reoccurrence of cancer is when it returns after it has been treated. When a cancer is diagnosed as not being related to cancer that was previously treated, it is called second cancer (American Cancer Society, 2020c). Second cancer may be found in the same area as the cancer you had before, or it could begin elsewhere (American Cancer Society, 2020d). Some of the risk factors that may lead to second cancer include tobacco use, excessive alcohol use and a lack of a follow-up after your first cancer was found. Ask your family care provider if you have factors that need more attention (American Cancer Society, 2020c). Both men and women can develop second cancer, but men have a higher chance of developing certain second cancers (American Cancer Society, 2020b). Some of these cancers include the prostate, small intestine and pancreas. Men need to see their family care provider regularly to look for any signs of reoccurrence or second cancers (American Cancer Society, 2020b). For further information on second cancer visit the Resources tab.
Adolescents and young adults with cancer
People that are aged 15 to 39 are considered in the adolescent and young adult category (National Comprehensive Cancer Network, 2022). People in these categories can have unique challenges that affect them, including concerns about fertility, employment, childcare and psychosocial aspects, such as mood and relationships with loved ones. The National Comprehensive Cancer Network (NCCN) (2022) recommends that certain vaccinations, including the HPV vaccine be given to those aged 9 to 26. There may be other vaccinations that are recommended for your age group, so it is important to ask your family care provider. The timing of vaccinations may also be important to consider based on when you completed your cancer treatment. Vaccines help to protect you against infection by giving your body the ability to respond to a disease. It is common to experience distress, depression and anxiety, so it is important to seek support from counsellors, peer support groups and your care team (NCCN, 2022). It can be hard to know what to say to people around you, so take your time to recover. It might be hard to concentrate at school, so lowering your course load may help, and plan to work on assignments for longer. Your care team can work with your school if side effects are getting in the way of your studies. For more information on adolescents and young adults please access the link for NCCN (2022) in the references (National Comprehensive Cancer Network, 2022).
2. Comprehend the domains of needs for patients living with cancer.
Cancer is an unexpected life event that can have tremendous significance to individuals and their families. These impacts are often much deeper than that of physical effects. Many clients face spiritual, emotional, and practical impacts that require assistance throughout their cancer journey. As patients progress through their cancer journey their needs can differ, this can be affected by the stage and intensity of the disease.
- Physical: The maintenance of physical comfort, pain, control, nutrition, and ability to engage in normal daily activities (Fitch, 2008). Examples such as pain, weakness, fatigue, anorexia, nausea & vomiting, mobility and lymphedema.
- Emotional: A sense of comfort, belonging, acceptance and encouragement during stress (Fitch, 2008). Examples such as fear, anxiety, depression, guilt, anger, powerlessness, isolation and sexuality concerns.
- Practical: Assistance related to tasks or activities that have to be carried out in everyday life (Fitch, 2008). Examples such as shopping, transportation, childcare, family relief, family stresses, financial issues, legal issues and home care activities.
- Informational: Information is required to reduce uncertainty, anxiety, and fear; to inform patient/family decision-making and to assist in skill attainment (Fitch, 2008). Examples such as procedures, educational sources, side effect management, treatment and assistance with decision-making.
- Spiritual: Meaning and purpose in one’s life (Fitch, 2008). Examples such as the search for meaning, spiritual crisis, practice of religious beliefs and existential despair.
- Social: Family relationships, community involvement, acceptance, and relationships (Fitch, 2008). Examples such as sharing with others, social relationships, family/children responses, role change and communication.
2.1 What are the phases of needs for patients living with cancer?
Phase 1 – Pre-diagnosis: During this stage, patients may be exhibiting symptoms and nervously waiting for test results from their doctors. (Fitch, 2008). In the pre-diagnosis phase, gaining information, education, and help accessing screening tests is critical.
Phase 2 – Diagnosis: During this stage, the patient will have numerous procedures and diagnostic tests. Many patients feel anxious and feel as if they have no control as they wait for results (Fitch, 2008). At the diagnosis stage, information, education, psychosocial support, additional testing, and follow-up appointments are required.
Phase 3 – Dialogue/referral: After being diagnosed with cancer, patients can feel incredibly stressed, fearful, panicked, and anxious. This is now an event in their life that will leave an incredible impact. This stage may be at the point where the patient shares their diagnosis with loved ones (Fitch, 2008). At the dialogue or referral stage, psychosocial support, Information, and education about the type of cancer are important.
Phase 4 – Treatment: An incredibly difficult decision is occurring during this stage. The patient and loved ones will take in information and education and choose a treatment plan that best suits them. They work with their healthcare team during this decision as well (Fitch, 2008). During treatment: Patients may feel difficult side effects that make it hard to complete activities of daily living. Possible treatment options may include surgery, chemotherapy, radiation, or immunotherapy (Fitch, 2008). In the treatment stage, information about each treatment option, education on coping with the side effects of treatment, and support are important.
Phase 5 – Rehabilitation: As patients try to create a new normal, they may have to reflect on their cancer journey and what alterations this left them with (Fitch, 2008). In rehabilitation phase, assessments, understanding, and support are important.
Phase 6 – Survivorship: Patients may have to deal with the long-term effects of treatment and may not be as healthy as peers their age (Fitch, 2008). In the survivorship phase, helping to live with long-term effects and creating a new normal is crucial.
Phase 7 – Recurrence: Cancer has returned (Fitch, 2008). At the recurrence phase, assessment, psychosocial support, connection to the healthcare team and testing are significant.
Phase 8 – Non-curative disease: Patients with a non-curative diagnosis may worry they have little time left and may begin to grieve what their future would have been (Fitch, 2008). In the non-curative disease phase, symptom management, emotional support, and caregiver support for anticipatory grief, and the importance of having wishes and goals met using the Serious Illness Conversation guidelines can be helpful to best identify what the client is wanting for the last months of their life. http://www.bccancer.bc.ca/new-patients-site/Documents/SeriousIllnessConversationGuideCard.pdf
Phase 9 – Final days: anticipatory grief may be present during this time. In the final days, comfort for the patient, and emotional support for the patient and loved ones are key areas (Fitch, 2008). Continuing to provide education, empathy and compassion on what is expected so that the family knows that their loved one is comfortable.
Phase 10 – Bereavement: This stage is primarily grief (Fitch, 2008) and includes support for emotional reactions to caregivers and family members.
Refer to the patient journey on
http://www.bccancer.bc.ca/our-services/centres-clinics/bc-cancer-vancouver/patient-journey (BC Cancer, 2024).
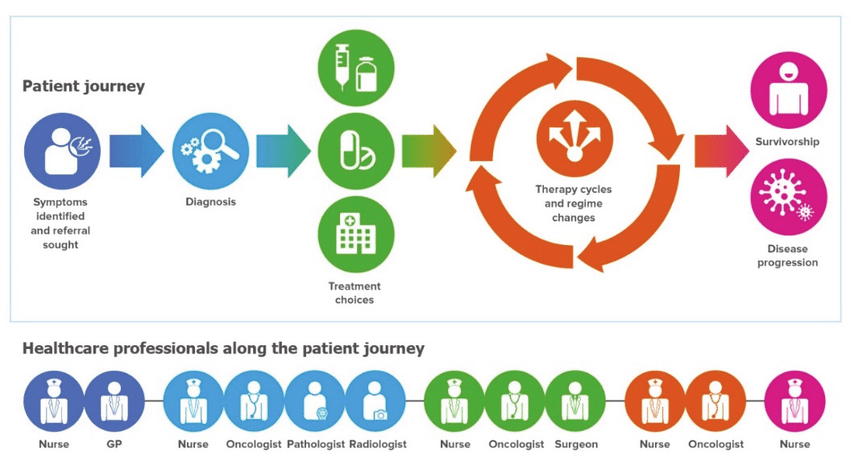
2.2 What is the pathway of a patient living with cancer?
The pathway of a patient with cancer can differ for each patient. Cancer is an incredibly complex and specific journey for each client and their route on this pathway can differ from patient to patient (Northwest Territories Health and Social Services, 2015).
- Prevention: health promotion of different lifestyle choices and information to prevent cancer from developing and information to decrease the likelihood of the development of cancer.
- Early detection and screening: mammograms, pap, and fecal immunochemical tests are examples of screening tests that are used in this stage of the pathway to catch non-symptomatic people who are at risk of developing cancer such as age and genetics.
- Diagnostic procedure: additional tests done to confirm a particular cancer or disease. The more tests that are performed the better understanding of the precise cancer the patient has and having different diagnostic testing completed can allow for an increased understanding as to where the cancer is located and the extent of disease.
- Diagnosis and staging: after the results of the diagnostic procedures, physicians and oncologists will determine the extent of the cancer in the body, and where it is located, and help or decide an appropriate treatment plan.
- Treatment: treatment varies on many different variables, such as the stage of cancer and the needs of patients. Treatment examples include chemotherapy, surgery, radiation therapy, immunotherapy, and hormonal treatments.
- Follow-up: can include appointments, and support programs to help patients transition to this stage.
- Palliative care: after discussion and progression of cancer is unable to be continually treated as well as conversation of a palliative approach based on the choice made by the client if not seeking active treatment.
- Survivorship: annual check-ups and support programs to help patients on how to live their life after cancer.
- Recurrence: diagnostic procedures to assess cancer status
- Transition to end of care: no procedures or interventions to treat cancer, this is about providing comfort to the patient during the end of their life.
(Northwest Territories Health and Social Services, 2015).
Refer to Clinical Care Pathways at http://www.bccancer.bc.ca/health-info/clinical-care-pathways (BC Cancer, 2024).
2.3 What is supportive care in cancer?
Supportive care in cancer can be defined as providing the necessary services to those who have cancer or have been affected by cancer to meet their physical, emotional, social, psychosocial, spiritual, practical, and informational needs (Fitch, 2008). This care also extends into navigating the phases of diagnostics, treatment, follow-up, survivorship, palliative care, and possibly bereavement (Fitch, 2008). This concept revolves around recognizing that patients with cancer and their families require additional services beyond medical interventions to support them and their ability to cope (Fitch, 2008). Supportive care must be tailored to each specific individual and their needs at each phase of their cancer journey (Fitch, 2008).
Refer to Supportive Care at http://www.bccancer.bc.ca/our-services/services/supportive-care (BC Cancer, 2024).
Refer to Support programs at http://www.bccancer.bc.ca/our-services/services/support-programs (BC Cancer, 2024).
2.4 What are the types of healthcare services in cancer care?
Types of Service
Types of services that may assist people living with cancer and the cancer care team members.
- Occupational Therapy: physical, cognitive, and affective impairments, to help restore functioning and provide appropriate equipment to ensure that the individual can continue to complete their daily activities while they are able. Helps avoid disability and encourages independence for daily activities of living (Cancer Care Alberta, 2022).
- Physiotherapy: focuses on the musculoskeletal system to provide person-centered rehabilitation (Cancer Care Alberta, 2022).
- Dietician: educate about nutrition and food, and use the extensive knowledge base to assess cancer patients’ nutrition to achieve optimal health and benefits (Cancer Care Alberta, 2022).
- Psychologist: psychosocial services to address emotional, cognitive, interpersonal, and developmental factors. They develop personalized care plans with flexibility to minimize risk and maximize treatment outcomes (Cancer Care Alberta, 2022).
- Social Worker: services patients and their families with supportive counselling, transitions, advocacy, and resources, addressing barriers to care (financial, shelter, transportation, employment) (Cancer Care Alberta, 2022).
- Respiratory therapist: provide insight into clients’ oxygen needs, assist with medication management, and make suggestions on respiratory care.
More information on types of services can be found on page 4 of the Supportive Care: Psychosocial and Rehabilitation Oncology, which is an adapted image from Fitch (2008).
Refer to our services at http://www.bccancer.bc.ca/our-services (BC Cancer, 2024).
Refer to services and support at http://www.bccancer.bc.ca/our-services/patient-guide/services-support (BC Cancer, 2024).
3. Explain the various roles of professional or health navigation.
Professional navigation was created and encouraged throughout Canada with the goals of decreasing gaps and addressing the specific needs of patients encountering complex situations, such as diseases (Canadian Partnership Against Cancer, 2012). Many programs have been created to introduce this role to various healthcare regions and are targeted at supporting clients from diagnosis to survivorship (Canadian Partnership Against Cancer, 2012). This role focuses on providing resources, information, emotional support, decision-making tools, practical assistance, and also providing community support (Canadian Partnership Against Cancer, 2012).
Refer to Indigenous Cancer Control http://www.bccancer.bc.ca/our-services/services/indigenous-cancer-control (BC Cancer, 2024).
The following video depicts what a cancer patient navigator’s role is and the type of support they provide to patients. It focuses on the importance of psychosocial support required in conjunction with clinical support to provide the most comfortable cancer journey possible for patients (Cable News Network [CNN], 2015).
3.1 What are the types of health navigation?
Patient navigation is working with and collaborating with a patient and their family to navigate through a disease or diagnosis including treatment, diagnostics, and other barriers through their journey through the medical system (Canadian Association of Nurses in Oncology [CANO], 2020).
Professional navigators are trained with a specific knowledge base in oncology and are part of a multidisciplinary team that focuses on person-centred care (Canadian Partnership Against Cancer, 2012). These navigators perform standard clinical assessments and introduction of interventions (Canadian Partnership Against Cancer, 2012).
Peer navigation: These navigators are trained peers and are sometimes paid for this position (Canadian Partnership Against Cancer, 2012). They are often a person with cancer experience themselves who can provide empowerment, support, and information about cancer and the journey to follow (Canadian Partnership Against Cancer, 2012). Peer navigators can be advocates for patients and can refer to healthcare services and other team members as needed (Canadian Partnership Against Cancer, 2012).
Virtual navigation: With the everchanging technology and the different barriers to accessing care, virtual navigation was piloted to see how web-based supports and communication techniques can be used to support cancer patients (Canadian Partnership Against Cancer, 2012). The research found that virtual navigation in web tools can help increase autonomy and empower patients during their cancer journey (Canadian Partnership Against Cancer, 2012).
Refer to Indigenous Health at http://www.phsa.ca/our-services/programs-services/indigenous-health#Programs–&–Services (Provincial Health Services, 2024).
3.2 What is the role of healthcare providers in cancer care?
- Family doctor: A general practitioner who can often help refer patients to specialists or diagnostic tests based on symptoms. Can provide support before, during, and after cancer treatment (Canadian Cancer Society, 2023).
- Oncologist: A doctor whose specialty is working to diagnose cancer and create treatment plans that are most appropriate for patients with cancer (Canadian Cancer Society, 2023).
- Oncology nurse: Specialized nurses with specific and extensive knowledge of cancer. Helps provide assessments, medications, treatment, and manage side effects (ONS, 2017).
- Social worker: services patients and their families with supportive counselling, transitions, advocacy, and resources, addressing barriers to care (financial, shelter, transportation, employment) (Cancer Care Alberta, 2022).
- Physiotherapist: focuses on the musculoskeletal system to provide person-centered rehabilitation (Cancer Care Alberta, 2022).
3.3 What is the role of nurses in cancer care?
Nurses are involved in educating the patient and their loved ones about their cancer and the specifics of their diagnosis (Cancer Care Alberta, 2022). Oncology nurses take part in all phases of need throughout a cancer journey such as prevention, screening, diagnosis, treatment, follow-up care, survivorship, rehabilitation, or possibly palliation (Cancer Care Alberta, 2022). Oncology nurses use information regarding cancer prevention and the importance of screening measures to help promote health. As well as this they possess the skills to assess and intervene effectively for cancer symptom management (Cancer Care Alberta, 2022).
Refer to Nursing. http://www.bccancer.bc.ca/health-professionals/clinical-resources/nursing (BC Cancer, 2024).
Summary
In knowledge hub 1 we discussed cancer and the role of professional navigators in providing patient support. The phases of need for cancer patients during each stage of their cancer journey were defined and recognized that this journey may not be exact for all patients. There are many different responsibilities of a navigator, all contributing to the goal of providing education, and support, and decreasing any barriers to care. Different types of navigators vary from patient, professional, virtual, and peer. Interdisciplinary and multidisciplinary healthcare team members can be involved in a patient’s cancer journey such as a doctor, nurse, or oncologist, each providing a specific knowledge base about each phase of cancer (Canadian Partnership Against Cancer, 2012; Fitch, 2008).
References
- Canadian Association of Nurses in Oncology [CANO/ACIO]. (2020). Patient Navigator in cancer care specialized oncology nurse role that contributes to high-quality, person-centered care experiences and clinical efficiencies. Can Oncol Nurs J , 30(3), 227-228.
- Canadian Cancer Society. (2023). Glossary. Retrieved from https://cancer.ca/en/cancer-information/resources/glossary
- Canadian Partnership Against Cancer. (2012). Navigation: A Guide to Implementing Person- Centered Care.
- Cancer Care Alberta. (2022). Supportive Care: Psychosocial and Rehabilitation Oncology.
- Cancer Fundamentals. (2019). BC Cancer: Provincial Health Services.
- Fitch, M. I. (2008). Supportive care framework. Can Oncol Nurs J , 18(1), 6-24. doi:10.5737/1181912×181614
- Government of Northwest Territories. (2020). Cancer Nurse Navigator Job Description.
- Northwest Territories Health and Social Services. (2015). Charting Our Course: Northwest Territories Cancer Strategy.
- Oncology Nursing Society [ONS]. (2017). Oncology Nurse Navigator Core Competencies. (ONS, 2017).
- Pfizer Oncology. (2018). Navigating the Cancer Continuum: in the context of Value- Bases Care.
Resources
- BC Cancer. (2024, April). Patient guide. Provincial Health Services Authority, BC Cancer, British Columbia. http://www.bccancer.bc.ca/our-services/patient-guide
- BC Cancer. (2024, April). patient journey. Provincial Health Services Authority, BC Cancer, British Columbia. http://www.bccancer.bc.ca/our-services/centres-clinics/bc-cancer-vancouver/patient-journey
- BC Cancer. (2024, April). Clinical Care Pathways. Provincial Health Services Authority, BC Cancer, British Columbia. http://www.bccancer.bc.ca/health-info/clinical-care-pathways
- BC Cancer. (2024, April). Supportive care. Provincial Health Services Authority, BC Cancer, British Columbia. http://www.bccancer.bc.ca/our-services/services/supportive-care
- BC Cancer. (2024, April). Support programs. Provincial Health Services Authority, BC Cancer, British Columbia. http://www.bccancer.bc.ca/our-services/services/support-programs
- BC Cancer. (2024, April). our services. Provincial Health Services Authority, BC Cancer, British Columbia. http://www.bccancer.bc.ca/our-services
- BC Cancer. (2024, April). services and support. Provincial Health Services Authority, BC Cancer, British Columbia. http://www.bccancer.bc.ca/our-services/patient-guide/services-support
- BC Cancer. (2024, April). Indigenous Cancer Control. Provincial Health Services Authority, BC Cancer, British Columbia. http://www.bccancer.bc.ca/our-services/services/indigenous-cancer-control
- Provincial Health Services. (2024, April). Indigenous health. Provincial Health Services Authority, British Columbia. http://www.phsa.ca/our-services/programs-services/indigenous-health#Programs–&–Services
- BC Cancer. (2024, April). Nursing. Provincial Health Services Authority, BC Cancer, British Columbia. http://www.bccancer.bc.ca/health-professionals/clinical-resources/nursing
-
BENEFITS OF PHYSIOTHERAPY ON THE CANCER PATIENT
-
Patient navigation
Videos
CNN. (2015, Jan 28). Cancer Patient Navigator. [Video]. Youtube. https://www.youtube.com/watch?v=YDa8Uea603g
Images
JourneyPure Rehab (2021). [Handshake-two people shaking hands]. Flickr. https://flic.kr/p/2kRNUHb )
Ivan Radic. (2020). [ Close-up of a Light Therapy Device and a physiotherapist in the background strapping his patient]. Flickr. https://flic.kr/p/2kf3xbQ ,

